Chlamydia treatment
Chlamydia treatment
Chlamydia treatment
- Effective treatment for chlamydia
- Take 1 tablet, twice a day, for 7 days
- Not suitable if you have chlamydia symptoms
What is chlamydia?
Chlamydia is a Sexually Transmitted Infection (STI) caused by the bacteria chlamydia trachomatis. It is the most common bacterial STI in the UK, and is usually transferred by having unprotected sex. In England, more than 64,000 people tested positive for the infection in 2023.
People can have chlamydia and not know about it, most people don't get any symptoms. That's why it spreads so easily. It can be very easily treated, but you can also reduce your risk of getting it by using condoms every time you have sex, particularly with a new partner.
Can you get rid of chlamydia?
Because chlamydia is a bacterial infection, it can easily be treated with a 7-day course of oral antibiotics. You need to take your antibiotics exactly as directed by your doctor.
In the UK the current gold standard treatment is a week's course of Doxycycline. This has a much higher cure rate than the alternative treatment Azithromycin. It's also important not to have any sex during your treatment and get all partners tested and treated.
How long does chlamydia last
It can take up to 14 days for chlamydia to show up in a test, so if you do the test too early after unprotected sex, it might come back negative. It's very rare for chlamydia to disappear on its own, if you have a positive test, you really do need to take treatment. Untreated chlamydia can lead to complications. Remember you are also likely to pass it on to any partners unless you have been treated. An uncomplicated infection is usually cured after seven days of treatment.
How to take chlamydia treatment
- Take 1 tablet, twice a day, for 7 days.
- Swallow the tablet with plenty of water.
- Doxycycline is best taken with food, or a glass of milk, and should be taken at least one hour before you go to bed.
- Complete the 7-day course of treatment to clear the infection.
- Do not have sex until you have completed all 7 days of treatment.
If you are allergic to Doxycycline, you may be prescribed an alternative antibiotic.
How effective is chlamydia treatment
When taken correctly, the prescribed treatment will kill the bacteria causing the infection. The NHS state that more than 95% of people with chlamydia will be cured when they take treatment correctly. You should avoid sexual contact until you and any sexual partners have completed the course of antibiotics.
This medicine is not a vaccination. You must take precautions to avoid reinfection. Using condoms every time you have sex (oral, vaginal, anal) is the best way to make sure you do not get STIs.
Chlamydia treatment side effects
The most common side effects include:
- Sensitivity to sunlight (exaggerated sunburn reaction)
- Indigestion (inflammation or ulcers of the gullet)
- Vaginal thrush (in women)
For full information on side effects and correct use, see the patient information leaflet. If any side effects concern you, contact us via your account.
How is chlamydia diagnosed?
Chlamydia can be tested for very easily. Because chlamydia is asymptomatic in so many people, it is essential to get screening if you have had a new partner. Chlamydia can be tested using a swab from the vagina or a urine sample, depending on the type of sex you have, a throat or rectal swab may also be recommended.
If you are aged between 15 and 24 it's a good idea to take part in the national chlamydia screening program. Anyone can get a free test kit through their GP surgery, local sexual health or contraception clinic.
When should you get tested for chlamydia?
If you’ve had unprotected sex or you think you might have been exposed to chlamydia or other STIs you should get tested as soon as possible. However, if it’s been less than two weeks since you had unprotected sex, you can still test but you may be asked to repeat the test two weeks after the unprotected sex to rule out chlamydia infection.
- You should regularly screen for STIs.
- For those at high risk, testing every three months is recommended.
- You can assess your risk of STIs using our free assessment.
- Chlamydia does not always come with symptoms so even if you feel completely healthy you may still be infected.
If you test positive for chlamydia, your partner must take treatment too. A test is usually recommended to confirm and check for other infections. You should not have sex until you and any partners have completed the treatment.
If you don’t have symptoms, you can order a discreet and easy-to-use home test kit for chlamydia for men, women, men who have sex with men, non- binary or trans people.
Complications of untreated chlamydia
Chlamydia usually doesn’t cause any symptoms. This is problematic because, when left untreated, chlamydia can potentially lead to serious health complications. The complications of chlamydia can include:
- Pelvic inflammatory disease - In women, untreated chlamydia can lead to pelvic inflammatory disease, which can in turn cause ectopic pregnancy, chronic pain, and even infertility.
- Inflammation in the testicles - In men, untreated chlamydia can cause inflammation in the testicles (orchitis) and/or inflammation in the tubes that carry sperm from the testicles (epididymitis). In some cases, this can lead to fertility problems.
- SARA - Occasionally chlamydia can cause inflammation of the joints. This is a type of arthritis called sexually acquired reactive arthritis (SARA). Most commonly the knee is affected, but other joints can also be involved. Some people who get this also get conjunctivitis.
How do you catch chlamydia?
Chlamydia is caused by the bacteria chlamydia trachomatis, it’s a bacterial infection and is carried within genital fluids (vaginal fluid, semen, pre-cum and rectal mucus). Chlamydia is primarily passed through unprotected sex (sex without a condom).
One of the sexual partners must already have chlamydia to pass on the infection. You can’t catch chlamydia without direct contact with the infection.
Chlamydia can be spread through:
- Vaginal sex
- Anal sex
- Oral sex
- Sharing sex toys
- Genital contact
- Genital fluids coming into contact with the eye
How to avoid catching chlamydia
“The best way to avoid chlamydia is to always use condoms when you aren’t certain that your partner is STI-free. It’s always a good idea to talk about your sexual history with a new sexual partner, including any recent STIs tests you might have had.” - Dr Bhavini Shah
- Use condoms correctly when you have vaginal or anal sex
- Use condoms to cover the penis during oral sex
- Dental dams can also be used for oral sex; these are thin, soft pieces of plastic or latex that are placed over the vagina or genital area
- Wash sex toys between uses or cover them with a fresh condom
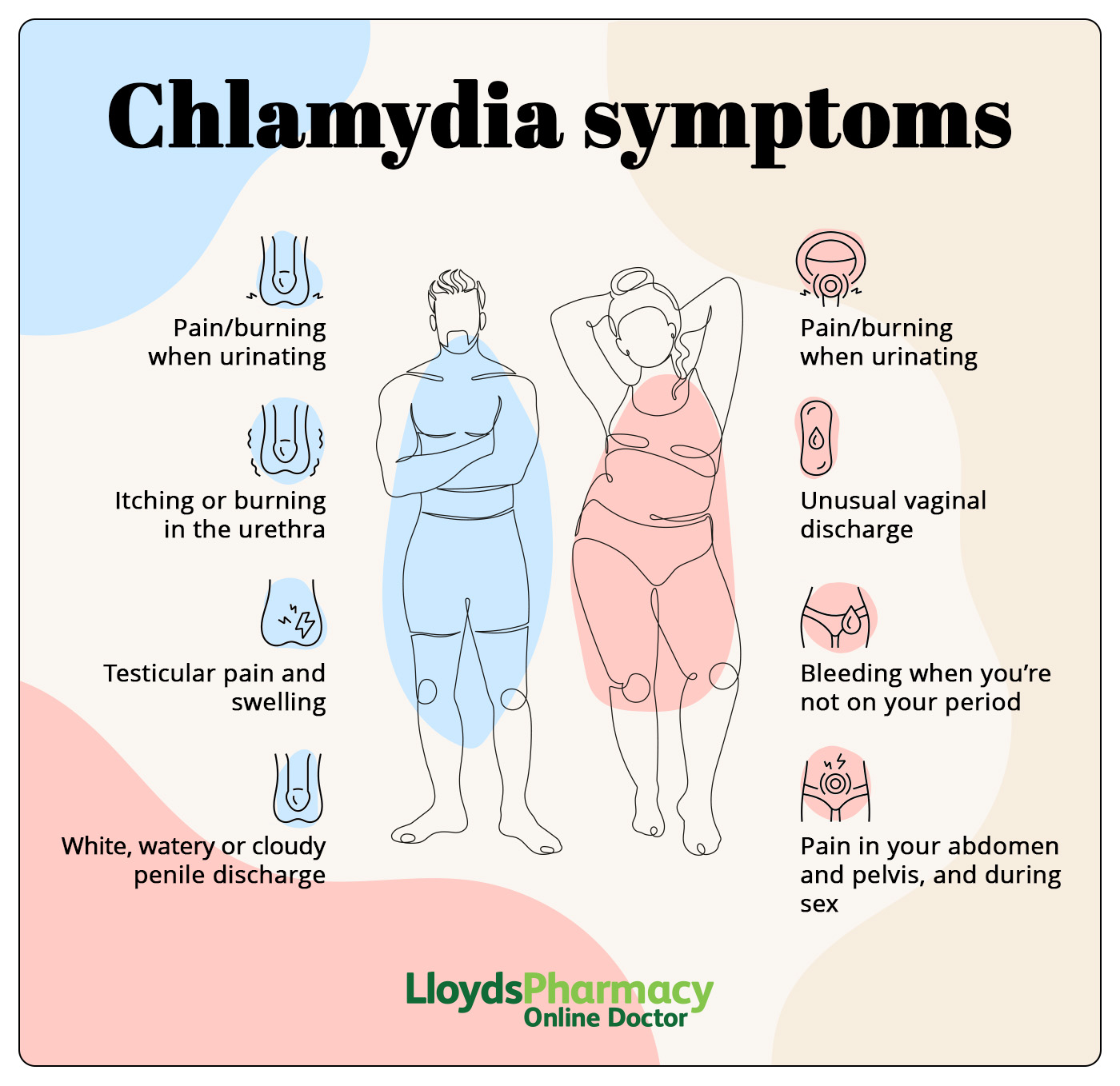
What are the symptoms of chlamydia?
Most people have chlamydia without knowing that they have it. However, some people do get symptoms. These can differ between men and women, which is why it’s a good idea to know what to look out for.
Penile chlamydia symptoms
- Discharge from penis which is white, cloudy or watery
- Burning sensation when urinating
- Epididymitis - painful swelling at the back of the testicle
Vaginal chlamydia symptoms
- Vaginal discharge that's different from your usual discharge
- Bleeding between periods/during or after sex
- Burning sensation when urinating
- Pelvic inflammatory disease (PID) - PID causes lower abdominal pain, vaginal discharge, fever and can affect fertility if left untreated.
If infected fluid has come into contact with the eye, you may develop conjunctivitis.
Can chlamydia be symptomless?
Chlamydia is notorious for its common lack of symptoms. The infection can easily be caught without realising.
At least 50% of men and up to 70% of women don’t notice any symptoms of chlamydia. If you have unprotected sex with a new partner, you should get an STI test regardless of how you might feel.



