Is it normal to have period pains?
Reviewed by Dr Bhavini Shah
Period pain is completely normal. Most people feel some degree of discomfort when menstruating. This pain feels like a bad tummy ache, but back pain and leg pain are also common.
Even though period pain is common, there are some things to be aware of. In this article we dive into the causes of painful periods, what’s abnormal and treatments available.
What causes period pain?
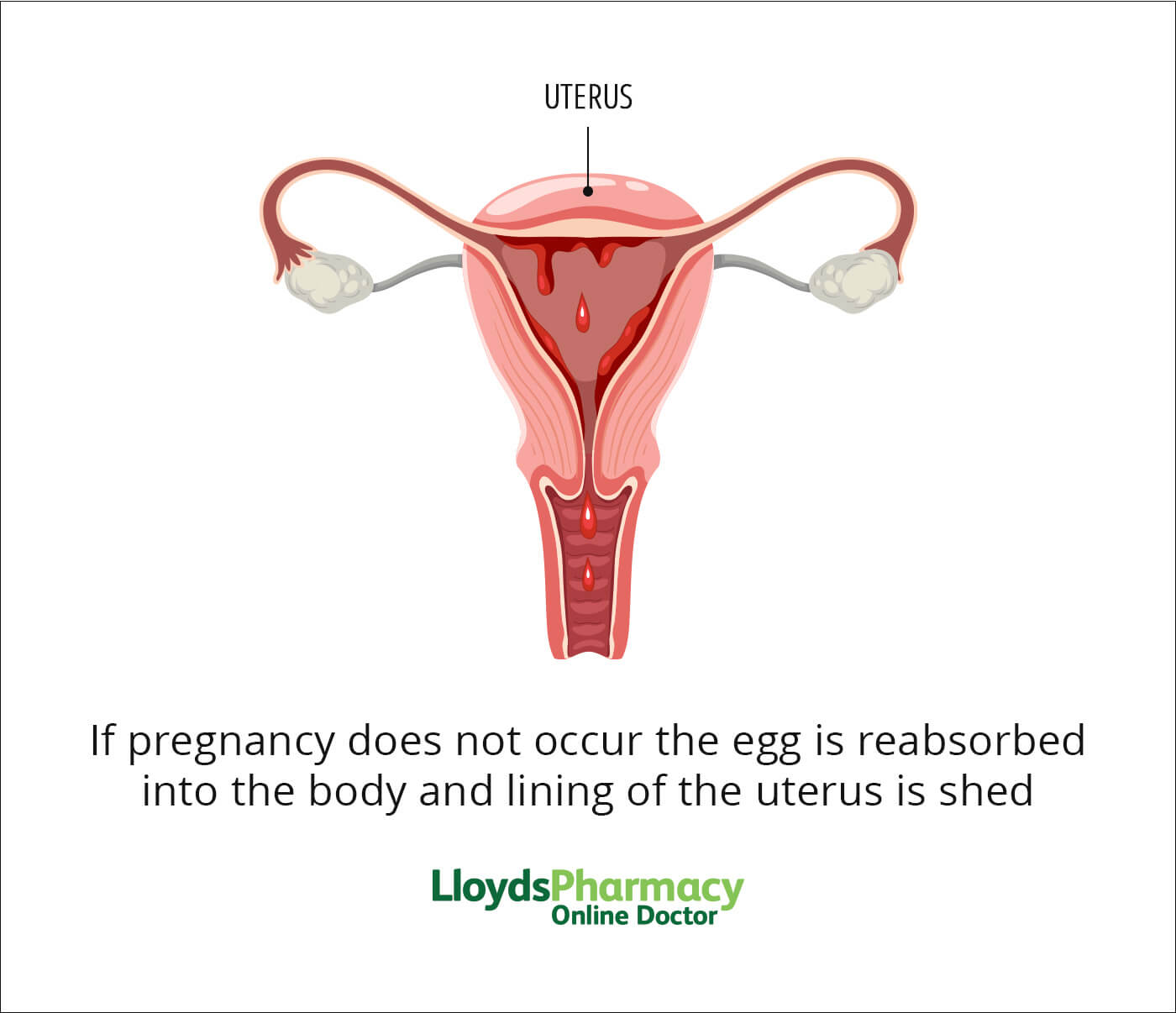
Period pain is caused by your womb (uterus) contracting to push out the uterine lining.
- Pain-triggering chemicals and prostaglandins are released
- The muscles in the womb contract
The build-up of prostaglandins or sensitivity to these may cause the womb to contract too hard. This reduces the blood supply to the womb and leads to pain. The more your womb contracts, the more pain you experience. If you suffer from unusually painful periods, then you should seek help from your GP in the first instance.
What health conditions can cause painful periods?
Sometimes intense period pain can be caused by an underlying health condition. They may need targeted medical treatment, if you’re concerned about your painful periods speak to your GP.
Common causes of bad period pain include:
- Endometriosis – this is where womb lining cells grow outside of the uterus, often on the fallopian tubes or ovaries. Endometriosis commonly causes pain throughout the month, becoming worse during your period.
- Fibroids – these are non-cancerous growths that develop inside the womb, causing heavy or painful periods, pain in the abdomen and back, and discomfort during sex.
- Pelvic inflammatory disease – this is an infection of the upper genital tract including the womb, fallopian tubes and ovaries that is almost always caused by a sexually transmitted infection such as chlamydia. Symptoms include pain in the abdomen and pelvis, pain during sex, abnormal vaginal discharge, and heavy, painful periods or irregular bleeding.
- Adenomyosis - this is where the tissue that normally lines the womb starts to grow within the muscular womb wall, making your periods particularly painful.
What are abnormal period pains?
Most women experience some form of period pains. Dysmenorrhoea refers to period pain, the term covers everything from dull aches to intense pain that isn’t manageable.
Abnormal levels of pain may stop you from doing everyday things like going to work or school. A study found that 1 in 4 women experience distressing menstrual pain which meant they needed medication to couldn’t carry on their usual daily activities. If the pain is affecting your daily life, you should see your GP.
You should seek treatment if:
- Your periods are also heavy or irregular
- Changes to your period pain
- The pain worsens or lasts for longer
- Pain at other times during your cycle
- You experience a feeling of heaviness in your tummy or back
“Painful periods or changes to the pain you experience during your periods could be a sign of a health condition, like endometriosis. It’s important to speak to your doctor if you have any worries. Especially if your pain is getting in the way of the things you enjoy.” - Dr Bhavini Shah
Treatment options for painful periods
If you’re struggling to cope with period pain, you shouldn’t suffer in silence. Health conditions that cause painful periods can be treated and managed in many ways.
Even if you don’t have an underlying health condition, there are still some options:
H3: Medical treatment
- Over-the-counter painkillers - ibuprofen and paracetamol are often effective
- Hormonal coil - many women find that their periods become lighter and less painful after having the hormonal coil fitted
- Combined contraceptive – this type of pill can help make periods lighter and less painful. This can be a good option even if you're sexually active.
- Mefenamic acid and Tranexamic acid - non-hormonal prescription treatments taken when your period is due on which help periods become lighter.
- Period delay treatment – could be used to delay your period for an event such as holidays or exams
Just remember that any noticeable changes in your menstrual cycle always warrant a visit to the GP.
Natural remedies for period pain:
- Exercise – releases endorphins which are natural painkillers
- Massage – may help to relax the uterine muscles
- Relaxation techniques can also be helpful
- Hot water bottles – applying heat to your lower stomach can help relieve cramps
- Warm shower or bath – can help you feel relaxed and ease cramps
Do contraceptives help with period pain?
Hormonal contraceptives can help some people with painful periods. The combined pill is one of the best contraceptives for period pain. It can help make periods lighter and less painful. It does this by preventing an egg being released (ovulation) and your uterus lining thickening.
It may take your body a while to adjust to the hormones in this pill. You may experience some cramping for the first few cycles. So, give your period time to settle before speaking to your GP about alternatives.
Other contraception options that can help with period pain are the implant and contraceptive injection. For some people these stop periods completely.
Conclusion
Period pain is a normal part of a lot of people’s periods. Although it can be uncomfortable there are there are ways you can manage menstrual pain. From painkillers, natural remedies to contraception like the combined pill or the implant. However, period pain can stop you from everyday activities and can be distressing. If your period pain is becoming unmanageable speak to your GP for advice.
References
https://www.nhs.uk/conditions/period-pain/
https://www.nhs.uk/conditions/periods/period-problems/
https://www.nhsinform.scot/healthy-living/womens-health/girls-and-young-women-puberty-to-around-25/periods-and-menstrual-health/period-pain-dysmenorrhoea/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3392715/






